Overview
The Eligibility page is comprised of three tabs:
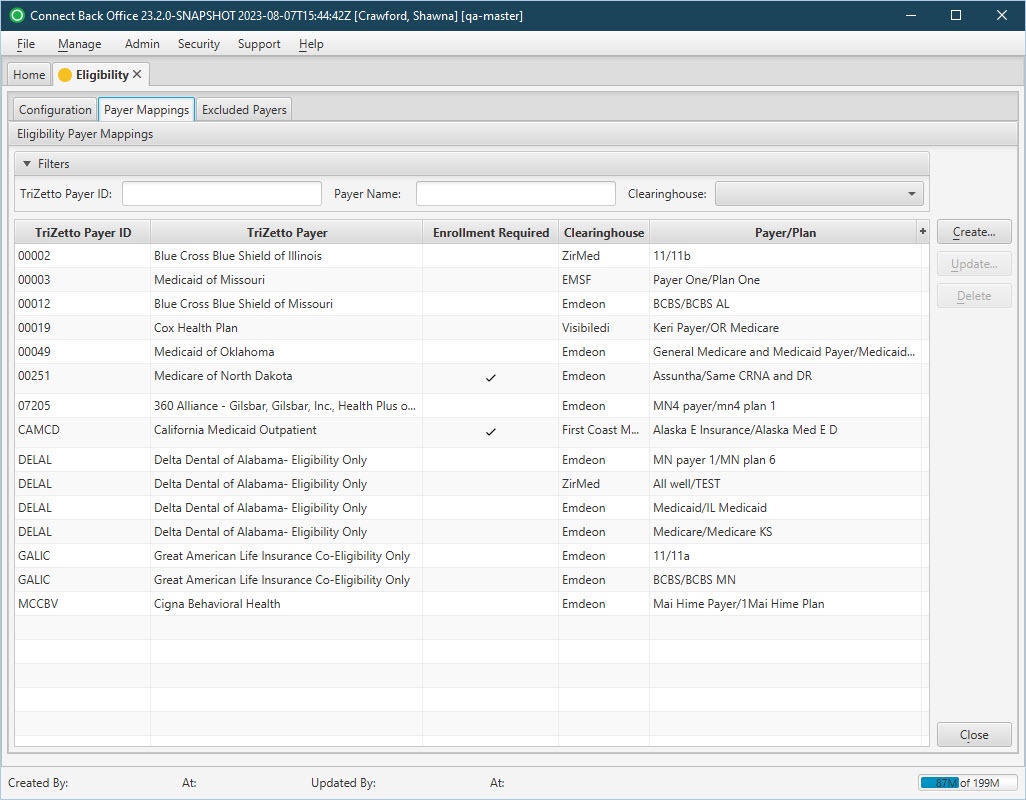
The Eligibility / Payer Mappings tab is used to view and map your full Eligibility payer list of TriZetto payers and their corresponding payer mappings. Eligibility requests are sent through the TriZetto clearinghouse. If you do not use the TriZetto clearinghouse, it will be necessary to map your clearinghouse payers/plans to a TriZetto Payer ID in order to use this functionality.
The tab also provides a quick view of which payers require additional enrollment.
Field Definitions
Field | Type | Required | Description |
|---|---|---|---|
| TriZetto Payer ID | Display Only (pulled from system) | Yes | The TriZetto Payer ID used by the TriZetto clearinghouse to identify the payer. |
| TriZetto Payer | Display Only (pulled from system) | Yes | The TriZetto Payer Name tied to the associate TriZetto Payer ID. |
| Enrollment Required | System-generated checkmark | No | Designation to identify if the Payer requires additional enrollment to use. |
| Clearinghouse | Display Only (pulled from created/updated Payer Mappings) | Yes | The name of the clearinghouse associated with payer/plan mapped to the TriZetto payer. |
| Payer/Plan | Display Only (pulled from created/updated Payer Mappings) | Yes | The name of the payer/plan mapped to the TriZetto payer. |
Button Descriptions
Button | Shortcut Keys | Description | Step-By-Step Guides |
|---|---|---|---|
| Create | [Alt] + [C] | Map a payer/plan to a TriZetto Payer ID. | Creating Payer Mappings |
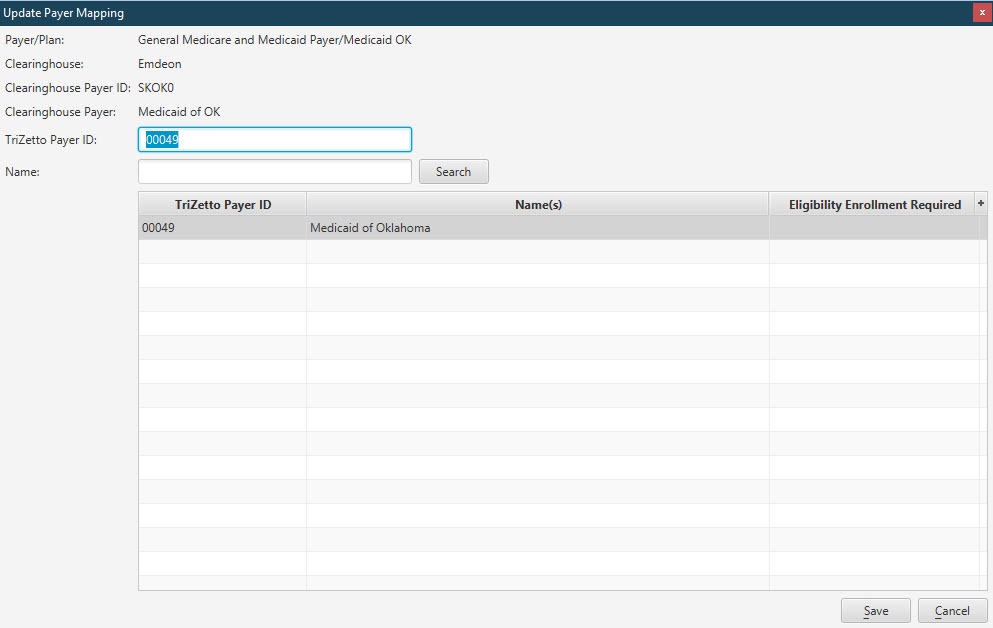
| Update | [Alt] + [U] | Update a payer/plan to TriZetto Payer mapping. |
|
| Delete | [Alt] + [D] | Remove a mapped payer/plan. |
|