Overview
Purpose
This report is used to review insurance plan configurations and demographic information.
Category
System
Type
Detail
Mode
Not applicable
Output Options
CSV or Excel
Sample Reports
(Click an image to enlarge)
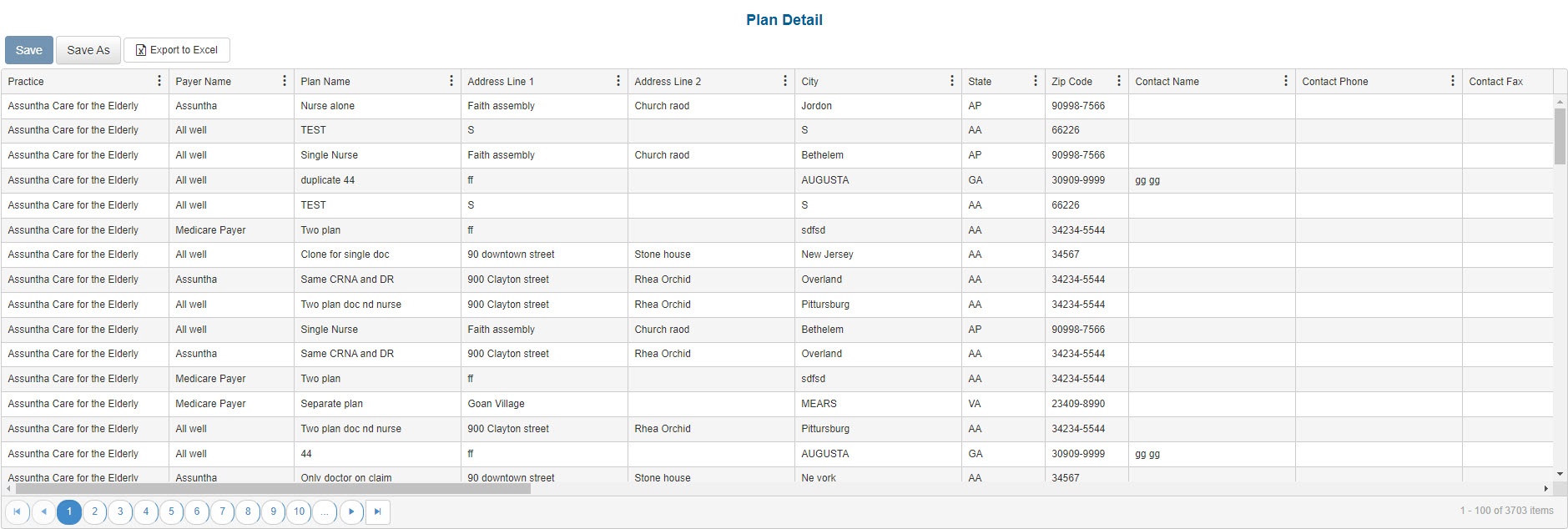
Portal
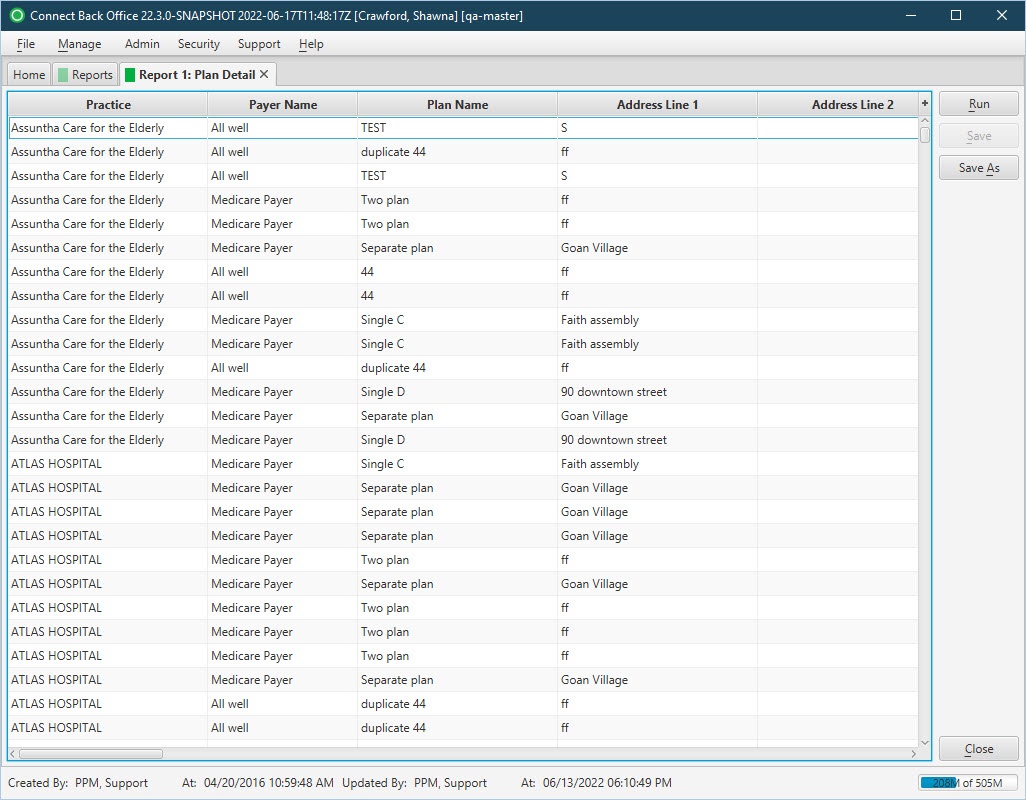
Back Office
Field Definitions
Field | Description |
|---|---|
| Practice | The name of the practice. |
| Payer Name | The name of the parent payer to the plan. |
| Plan Name | The name of the plan. |
| Address Line 1 | The address line 1 of the street address of the plan. |
| Address Line 2 | The address line 2 of the street address of the plan. |
| City | The city of the plan. |
| State | The state of the plan. |
| Zip Code | The postal ZIP code of the plan. |
| Contact Name | The name of the primary contact for the plan. |
| Contact Phone | The 10-digit telephone number of the primary contact for the plan. |
| Contact Fax | The 10-digit facsimile number for the plan. |
| Contact Email | The electronic email address of the primary contact for the plan. |
| Website | The URL to the website for the plan. |
| Financial Class | Indicates the grouping the plan on the case is in. Financial class is used for reporting purposes. For example, you can set up either a managed care financial class or a more detailed break down delineating PPO and HMO classifications. |
| Clearinghouse | The name of the associated clearinghouse that distributes claims to the correct insurance payer. |
| Payer ID | The unique identification number of the plan for the clearinghouse. |
| Claim Type | The abbreviation that identifies the type of claims that will be generated for the plan, for example, Automobile Medical (AM), Commercial Insurance Company (CI), Disability and Health Maintenance Organization (HM). |
| Billing Provider Type | The provider type who is the billing provider when claims are generated. |
| Team Billing | The type that identifies whether claims include charges for a physician and a CRNA when involved on the same case that results in team billing. Claims can include charges for the physician only or the physician and CRNA, or the physician or CRNA. |
| Concurrency Scheme Name | The name of the concurrency scheme selected for the plan. |
| Extreme Age | Indicates whether the plan allows the extreme age modifier. |
| Emergency | Indicates whether the plan allows the emergency condition modifier. |
| Primary Claim Type | The primary claim format for the plan, e.g., Electronic, Drop to Paper, Self-Print. |
| Secondary Claim Type | The non-primary claim format for the plan, e.g., Electronic, Drop to Paper, Self-Print. |
| Paper Claim Form | The claim format used for paper submission of claims on the plan. |
| Effective Date | The effective date of the plan. |
| Expiration Date | The expiration date of the plan. |
| Network Status | Provides quick identification if the plan is in or out-of-network. |
| Contract Effective Date | The date the provider begins accepting the plan. |
| Inactive | A "Yes/No" flag to indicate if the plan is currently active. |
| Billed Fee Schedule | The name of billing fee schedule on the plan. |
| Expected Fee Schedule | The name of the expected fee schedule on the plan. |
Available Report Filters
Option | Type | Required | Description |
|---|---|---|---|
| Practices | List Selection | No | Filters by one or more practices. By default, this filter is set to All. Only active practices are returned in the search results. |
| Payers | List Selection | No | Filters by one or more payers. By default, this filter is set to All. |
| Plans | List Selection | No | Filters by one or more plans. By default, this filter is set to All. |
| Report Folder | Drop Down | Yes | Designates where to place or save the output from the executed report. |