Overview
Purpose
This report analyzes elapsed time ranges between key milestones in the billing process. It is used to monitor activity on charges from the time a charge is received at your practice corporation, to when it is entered into the billing system, and then when it is paid by the insurance payer or guarantor.
Category
Management
Type
Detail
Mode
Date of Service
Output Options
CSV or Excel
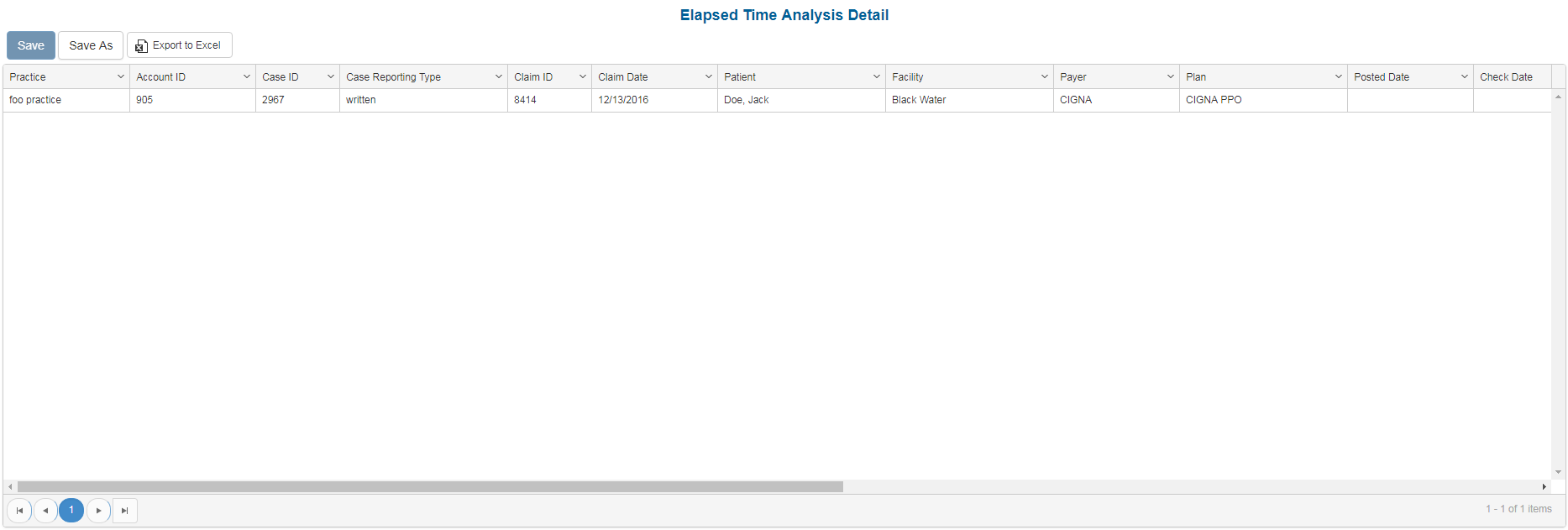
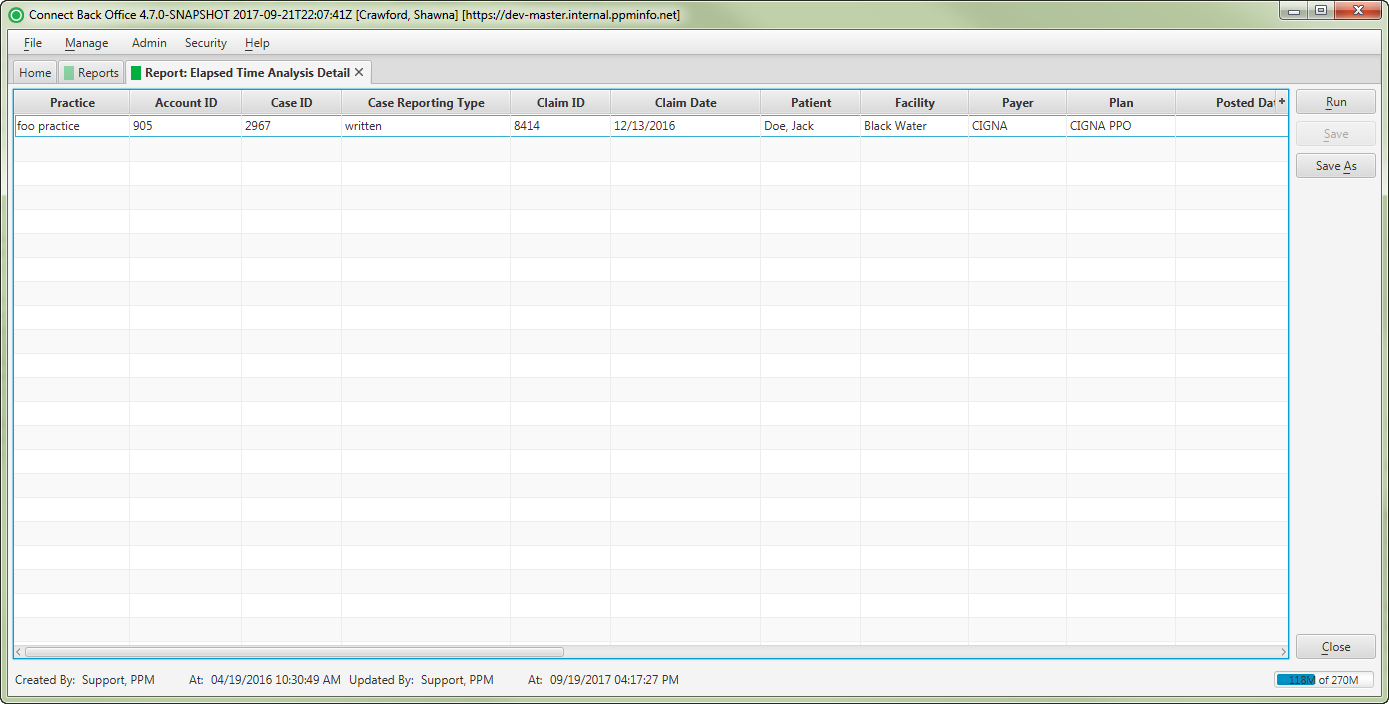
Sample Reports
(Click an image to enlarge)
Portal
Back Office
Field Definitions
Field | Calculation Formula | Description |
|---|---|---|
| Practice | The practice for which the charge is being billed. | |
| Account ID | The account number of the guarantor account. Displays as Account Prefix + Account ID. | |
| Case ID | The unique number assigned to the case. | |
| Case Reporting Type | The unique code assigned to the case for identifying the case for reporting purposes. | |
| Claim ID | The identification number issued to the claim when it was generated. | |
| Claim Date | The date that the claim was generated. | |
| Patient | The name of the patient. | |
| Facility | The name of the facility where services were rendered. | |
| Payer | The primary insurance payer on the case with financial responsibility for the outstanding debt. | |
| Plan | The primary insurance plan on the case to which charges were billed. | |
| Posted Date | The date the transaction was posted to the guarantor account. | |
| Check Date | The date of the check. | |
| Date of Service | The date the service is rendered. | |
| Billed | The total amount billed for each procedure on the case. | |
| ASA Code | The anesthesia procedure code that was entered as the procedure billed on the case in charge entry. | |
| CPT Code | The general procedure code that was entered as the procedure billed on the case in charge entry. | |
| Balance | The balance of the service line. | |
| Insurance Payments | All payments applied as Insurance Payments from the insurance company. | |
| Guarantor Payments | All payments applied as Guarantor Payments from the patient or guarantor. | |
| Total Payments | Total payments from the patient/guarantor or insurance. | |
| Claim Date/Check Date | Check Date - Claim Date | The number of days between the claim date and the check date. |
| Claim Date/Post Date | Claim Date - Post Date | The number of days between the posted date and the claim date. |
| DOS/Check Date | Check Date - Date of Service | The number of days between the check date and the date of service. |
| DOS/Claim Date | Claim Date - Date of Service | The number of days between the claim date and the date of service. |
| DOS/Post Date | Post Date - Date of Service | The number of days between the post date and the date of service. |
| Received Date/Claim Date | Claim Date - Received Date | The number of days between the received date and the claim date. |
| Received Date/Check Date | Check Date - Received Date | The number of days between the received date and the check date. |
| Received Date/DOS | DOS - Received Date | The number of days between the received date and the date of service. |
| Received Date/Post Date | Post Date - Received Date | The number of days between the received date and the post date. |
Available Report Filters
Results can be returned for one or more of the filter criteria (e.g., multiple practices).
Option | Type | Required | Description |
|---|---|---|---|
| Date | Drop Down | Yes | Filters transactions displayed by the selected time period. Options include: Custom Date Range, Last # of Days, Today, Previous Day, Current Month, Previous Month, Current Year, and Previous Year. By default, this filter is set to Current Month. If Custom Date Range is selected, the From and To fields are enabled to enter specific dates to run the query on. If Last # of Days is selected, the Last # of Days field is enabled to enter a specific number of days to run the query on. The maximum timespan for the report is 31 days. |
| Practices | List Selection | No | Filters by all practices or one or more practices for which charges were billed. By default, this filter is set to All. Only active practices are returned in the search results. |
| Facilities | List Selection | No | Filters by all facilities or by one or more facilities where services were rendered. By default, this filter is set to All. |
| Payers | List Selection | No | Filters by payer(s) to which claims were submitted. By default, this filter is set to All. |
| Plans | List Selection | No | Filters by plan(s) to which claims were submitted. By default, this filter is set to All. |
| Report Folder | Drop Down | Yes | Designates where to place or save the output from the executed report. |